News
Newswise —
FINDINGS
Researchers from the David Geffen School of Medicine at UCLA found that cardiovascular disease patients who have high muscle mass and low fat mass have a lower mortality risk than those with other body compositions. The findings also suggest that regardless of a person’s level of fat mass, a higher level of muscle mass helps reduce the risk of death.This findings indicate the importance of assessing body composition as a way to help predict cardiovascular and total mortality in people with cardiovascular disease.
BACKGROUND
In previous studies on the relationship between body composition and mortality, the researchers used a simpler clinical measure of body composition called the bio electrical impedance scale. They noted a possible protective effect of muscle mass on both mortality and metabolism in healthy people. The new study extends the findings from the earlier research using dual X-ray absorptiometry, a more rigorous method of measuring body composition.The researchers examined data from the National Health and Nutrition Examination Survey, 1999 to 2004, of 6,451 participants who had prevalent cardiovascular disease. Each subject was categorized into one of four groups:
low muscle/low fat mass
low muscle/high fat mass
high muscle/low fat mass
high muscle/high fat mass
Those with high muscle mass and low fat mass had the lowest risk of cardiovascular and total mortality.
IMPACT
Because people with higher muscle mass were more likely to have a high body mass index, the findings could explain the “obesity paradox,” which holds that people with a higher BMI have lower mortality levels. The findings also highlight the importance of maintaining muscle mass, rather than focusing on weight loss, in order to prolong life, even in people who have a higher cardiovascular risk. The authors suggest that clinicians encourage their patients to participate in resistance exercises as a part of healthy lifestyle changes, rather than focusing primarily on, and monitoring, weight loss.
AUTHORS
Dr. Preethi Srikanthan, associate clinical professor of medicine in the division of endocrinology at the David Geffen School of Medicine, is the study’s primary investigator. The study’s co-authors are Dr. Tamara Horwich, health sciences clinical professor of medicine, division of cardiology, and Dr. Chi-hong Tseng, adjunct associate professor of medicine in the division of general internal medicine and health services research.
JOURNAL
The study was published in the American Journal of Cardiology.
Newswise —
Catherine Aaron and Gabrielle Beaudry were 17 when they knocked on the door of the laboratory of Alex Parker, a neuroscience researcher at the University of Montreal Hospital Research Centre (CRCHUM). While students at Collège Jean-de-Brébeuf in Montreal, they were looking for a mentor for an after-school research project. Two and half years later, the results of this scientific adventure were published today in the Journal of Agricultural and Food Chemistry.
"We wanted to test the effect of a natural product on a neurodegenerative disease such as Alzheimer's. Professor Parker had already discovered that sugar prevents the occurrence of amyotrophic lateral sclerosis (ALS) in an animal model of the disease, the C. elegans worm. That’s how we got the idea of maple syrup, a natural sugar produced in Quebec,” said Beaudry.
Supervised by PhD student Martine Therrien and Alex Parker, Aaron and Beaudry added maple syrup to the diet of these barely 1 mm-long nematodes. "We just gave them a supplement of maple syrup at various concentrations and compared with a control group that had a normal diet," said Aaron. “After twelve days, we counted under the microscope the worms that were moving and those that were paralyzed. The worms that had consumed the highest dose of syrup were much less likely to be paralyzed.”
Alex Parker's C. elegans worms are genetically modified to express a protein involved in ALS in motor neurons – TDP-43. "When they are adults, around 12 days, their motor neurons break down. Normally, at two weeks of life, 50% of the worms are completely paralyzed. But among those that received a diet enriched with 4% maple syrup, only 17% were paralyzed. We can therefore conclude that maple syrup protects neurons and prevents the development of amyotrophic lateral sclerosis in C. elegans worms," said Parker, a researcher at the CRCHUM and professor at the Faculty of Medicine, University of Montreal.
How can we explain this dramatic effect? "Sugar is good for the nervous system. Diseased neurons require more energy to combat toxic proteins. But maple syrup is rich in polyphenols, powerful antioxidants found in certain foods. We isolated phenols contained in the maple syrup, and we showed that two polyphenols in particular, gallic acid and catechol, have a neuroprotective effect. In pure maple syrup, these polyphenols are found in low concentrations. Probably a combination of sugar and polyphenols prevents the occurrence of the disease in worms," said Therrien, a PhD student at the CRCHUM.
But don’t go ahead and gorge yourself on maple syrup thinking it'll protect you against neurological diseases! "The life expectancy of C. elegans worms is only three weeks. They are spared the long-term toxic effects of sugar. Humans who consume comparable amounts of sugar risk developing chronic diseases such Type 2 diabetes and obesity,” cautioned Parker.
Amyotrophic lateral sclerosis is a rare neuromuscular disease that causes paralysis and death a few years after the onset of symptoms. So far, no cure is available for patients. This latest study on maple syrup and the C. elegans worm was conducted for educational purposes. Other studies by Alex Parker with C. elegans have led to the discovery of promising drugs, which will be tested in patients in a few years.
Catherine Aaron and Gabrielle Beaudry won the Sanofi Biogenius Canada People’s Choice Award – Quebec section – for this project in April 2014. Aaron is now a first-year medical student at the University of Montreal, and Beaudry studies psychology at the University of Sherbrooke.
Newswise —
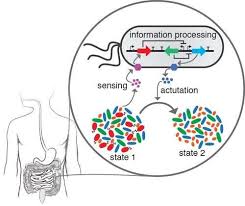
Researchers have shown that various types of intestinal bacteria might be factors in both causing and preventing obesity, and in other conditions and diseases. Now, a UCLA study suggests that it could also potentially be used to reduce the risk for some types of cancer.
The research, published online April 13 in the peer-reviewed journal PLOS ONE, offers evidence that anti-inflammatory “health beneficial” gut bacteria can slow or stop the development of some types of cancer.
Ultimately, doctors might be able to reduce a person’s risk for cancer by analyzing the levels and types of intestinal bacteria in the body, and then prescribing probiotics to replace or bolster the amount of bacteria with anti-inflammatory properties, said Robert Schiestl, professor of pathology, environmental health sciences and radiation oncology at UCLA and the study’s senior author.
“It is not invasive and rather easy to do,” he said.
Over millions of years, gut bacteria have evolved into both good and bad types: The good ones have anti-inflammatory properties and the bad ones promote inflammation. The human body typically contains about 10 trillion bacterial cells, compared with only 1 trillion human cells.
Schiestl and his colleagues isolated a bacterium called Lactobacillus johnsonii 456, which is the most abundant of the beneficial bacteria, and which has some pretty useful applications outside of medicine. “Since it is a Lactobacillus strain, it makes excellent yogurt, kefir, kombucha and sauerkraut.”
In the UCLA study the bacterium reduced gene damage and significantly reduced inflammation — a critical goal because inflammation plays a key role in many diseases, including cancer, neurodegenerative diseases, heart disease, arthritis and lupus, and in the aging process.
Previous research led by Schiestl presented the first evidence of a relationship between intestinal microbiota and the onset of lymphoma, a cancer that originates in the immune system. The new study explains how this microbiota might delay the onset of cancer, and suggests that probiotic supplements could help keep cancer from forming.
For both studies, Schiestl and his team used mice that had mutations in a gene called ATM, which made them susceptible to a neurologic disorder called ataxia telangiectasia. The disorder, which affects 1 in 100,000 people, is associated with a high incidence of leukemia, lymphomas and other cancers.
The mice were divided into two groups — one that was given only anti-inflammatory bacteria and the other that received a mix of inflammatory and anti-inflammatory microbes that typically co-exist in the intestines.
In the Cancer Research paper, Schiestl and his team showed that in the mice with more of the beneficial bacteria, the lymphoma took significantly longer to form.
In the new study, the researchers analyzed the metabolites — molecules produced by the gut’s natural metabolic action — in the mice’s urine and feces. The scientists were surprised to find that the mice that were receiving only the beneficial microbiota produced metabolites that are known to prevent cancer. Those mice also had more efficient fat and oxidative metabolism, which the researchers believe might also lower the risk for cancer.
Among the other results, in the mice receiving only the good bacteria, lymphoma formed only half as quickly as it did in the other mice. In addition, mice with the good bacteria lived four times longer and had less DNA damage and inflammation.
“Together, these findings lend credence to the notion that manipulating microbial composition could be used as an effective strategy to prevent or alleviate cancer susceptibility,” the researchers write. “Remarkably, our findings suggest that composition of the gut microbiota influence and alter central carbon metabolism in a genotype independent manner. In the future, it is our hope that the use of probiotics-containing [supplements] would be a potential chemopreventive for normal humans, while the same type of microbiota would decrease tumor incidence in cancer susceptible populations.”
Newswise —
Have you had the experience of being just on the verge of saying something when the phone rang? Did you then forget what it is you were going to say? A study of the brain’s electrical activity offers a new explanation of how that happens.
Published in Nature Communications, the study comes from the lab of neuroscientist Adam Aron at the University of California San Diego, together with collaborators at Oxford University in the UK, and was led by first author Jan Wessel, while a post-doctoral scholar in the Aron Lab. The researchers suggest that the same brain system that is involved in interrupting, or stopping, movement in our bodies also interrupts cognition – which, in the example of the phone ringing, derails your train of thought.
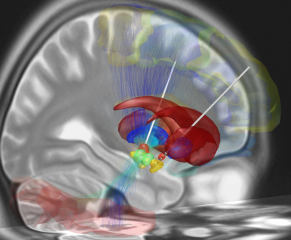
The findings may give insights into Parkinson’s disease, said Aron, a professor of psychology in the UC San Diego Division of Social Sciences, and Wessel, now an assistant professor of psychology and neurology at the University of Iowa. The disease can cause muscle tremors as well as slowed-down movement and facial expression. Parkinson’s patients may also present as the “opposite of distractible,” often with a thought stream so stable that it can seem hard to interrupt. The same brain system that is implicated in “over-stopping” motor activity in these patients, Aron said, might also be keeping them over-focused. The current study focuses particularly on one part of the brain’s stopping system – the subthalamic nucleus (STN). This is a small lens-shaped cluster of densely packed neurons in the midbrain and is part of the basal ganglia system.
Earlier research by Aron and colleagues had shown that the STN is engaged when action stopping is required. Specifically, it may be important, Aron said, for a “broad stop.” A broad stop is the sort of whole-body jolt we experience when, for example, we’re just about to exit an elevator and suddenly see that there’s another person standing right there on the other side of the doors.
The study analyzes signals from the scalp in 20 healthy subjects as well as signals from electrode implants in the STN of seven people with Parkinson’s disease. (The STN is the main target for therapeutic deep brain stimulation in Parkinson’s disease.)
All the volunteers were given a working memory task. On each trial, they were asked to hold in mind a string of letters, and then tested for recall. Most of the time, while they were maintaining the letters in mind, and before the recall test, they were played a simple, single-frequency tone. On a minority of trials, this sound was replaced by a birdsong segment – which is not startling like a “bang!” but is unexpected and surprising, like a cell phone chirping suddenly. The volunteers’ brain activity was recorded, as well as their accuracy in recalling the letters they’d been shown.
The results show, the researchers write, that unexpected events manifest the same brain signature as outright stopping of the body. They also recruit the STN. And the more the STN was engaged – or the more that part of the brain responded to the unexpected sound – the more it affected the subjects’ working memory and the more they lost hold of what they were trying to keep in mind.
“For now,” said Wessel, “we’ve shown that unexpected, or surprising, events recruit the same brain system we use to actively stop our actions, which, in turn, appears to influence the degree to which such surprising events affect our ongoing trains of thought.”
A role for the STN in stopping the body and interrupting working memory does fit anatomical models of how the nucleus is situated within circuitry in the brain. Yet more research is needed, the researchers write, to determine if there’s a causal link between the activity observed in the STN and the loss in working memory.
“An unexpected event appears to clear out what you were thinking,” Aron said. “The radically new idea is that just as the brain’s stopping mechanism is involved in stopping what we’re doing with our bodies it might also be responsible for interrupting and flushing out our thoughts.”
A possible future line of investigation, Aron said, is to see if the STN and associated circuitry plays a role in conditions characterized by distractibility, like Attention Deficit Hyperactivity Disorder. “This is highly speculative,” he said, “but it could be fruitful to explore if the STN is more readily triggered in ADHD.”
Wessel added: “It might also be potentially interesting to see if this system could be engaged deliberately – and actively used to interrupt intrusive thoughts or unwanted memories.”
If further research bears out the connection suggested by the current study, between the STN and losing your train of thought following an unexpected event, the researchers say it might be that it is an adaptive feature of the brain, something we evolved long ago as a way to clear our cognition and re-focus on something new. Aron suggests this example: You’re walking along one morning on the African Savannah, going to gather firewood. You’re daydreaming about the meal you’re going to prepare when you hear a rustle in the grass. You make a sudden stop – and all thoughts of dinner are gone as you shift your focus to figure out what might be in the grass. In this case, it’s a good thing to forget what you had been thinking about.
Newswise —
Expert: Frank Leone, MD, chair of the Tobacco Action Committee of the American Thoracic Society and noted expert in tobacco use treatment and smoking cessation.
The CDC’s latest report on tobacco use among teens between 2011 and 2015 showed decreased use of traditional tobacco products and significant increase in the use of e-cigarettes.
Frank Leone, MD, chair of the ATS Tobacco Action Committee, believes the misconception that e-cigarettes are safer than traditional cigarettes is driving the trend to increased use, which puts children and other first-time users at risk for significant health problems.
Key Messages:• There are risks associated with liquid nicotine, including addiction.• Studies have shown that the mechanical and chemical characteristics of e-cigarettes contribute to potentially hazardous health effects.• Chemicals in the liquid nicotine flavorings are particularly dangerous for children, and one study showed that flavorings altered lung function at the cellular level.
The CDC report states that “if current smoking rates continue, 5.6 million Americans aged <18 years who are alive today are projected to die prematurely from smoking-related disease.”
“That’s not only a cause for great concern,” said Dr. Leone. “It’s a call to action. President Obama and the FDA need to lead the charge now by regulating e-cigarettes and all tobacco products.
Newswise —
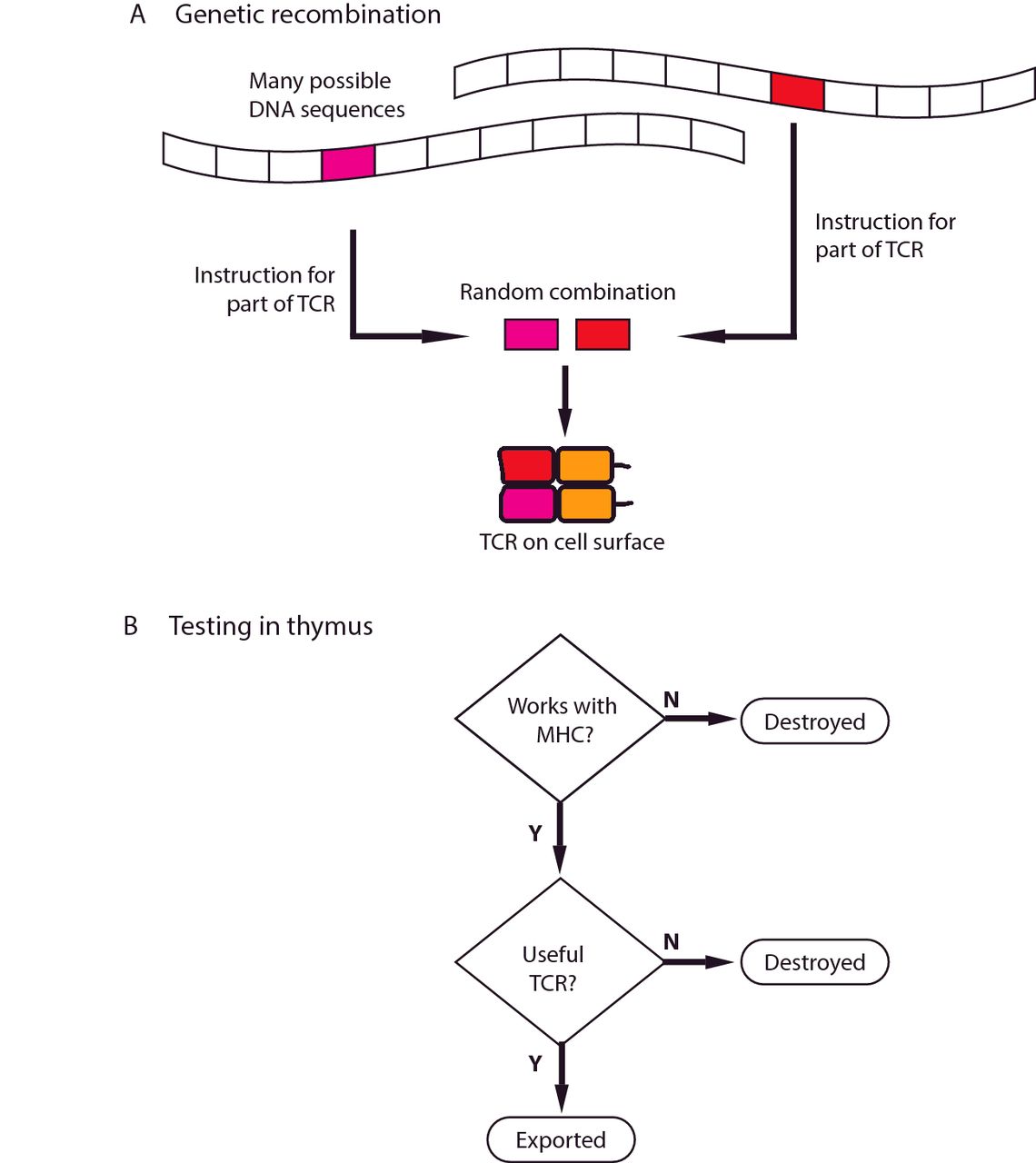
The fates of immune cells can be decided at the initial division of a cell. Researchers at St. Jude Children’s Research Hospital have discovered that the production of daughter cells with different roles in the immune system is driven by the lopsided distribution of the signaling protein c-Myc. Nudging c-Myc in one direction or the other could make vaccines more effective or advance immunotherapies for cancer treatment. The research appears online today in the scientific journal Nature.
Asymmetric cell division generates two types of cells with distinct properties. This type of cell division is essential for producing various cell types and plays an important role in development. Rather than producing two identical daughter cells, the cells undergoing asymmetric division produce daughter cells that are fated for vastly different roles. In the case of activated T cells, researchers knew that one daughter cell became the rapidly dividing effector T cells that launch the immediate attack on infectious agents and other threats. The other daughter cell became the slowly dividing memory T cells that function like sentries to provide long-term protection against recurring threats. Until now, the mechanism underlying the process was unknown.
“Our study shows that the way in which the regulatory protein c-Myc distributes during asymmetric cell division directly influences the fate and roles of activated T cells,” said corresponding author Douglas Green, Ph.D., St. Jude Department of Immunology chair. “We also show how this asymmetry is established and sustained.”
The researchers worked with cells growing in the laboratory and in mice. Scientists showed that during asymmetric cell division of activated T cells, high levels of c-Myc accumulated in one daughter cell. There, c-Myc functioned like a shot of caffeine to launch and sustain the rapid proliferation of effector T cells, including those in mice infected with the influenza virus. In contrast, the daughter cells with low levels of c-Myc functioned like memory T cells, proliferating to mount an immune response a month later when mice were again exposed to the virus.
Researchers also identified the metabolic and signaling pathways that serve as a positive feedback loop to sustain the high levels of c-Myc that effector T-cells require to maintain their identities and function. The scientists showed that disrupting certain components of the system disturbed c-Myc production, which altered the fate of T cells and caused effector T cells to operate like memory T cells.
“Our work suggests that it may be possible to manipulate the immune response by nudging production of c-Myc in one direction or the other,” Green said. “Potentially that could mean more effective vaccines or help to advance T-cell immune therapy for cancer treatment.”
c-Myc is an important transcription factor that regulates expression of a variety of genes and plays a pivotal role in cell growth, differentiation and death via apoptosis (programmed cell death). Excessive or inappropriate production of c-Myc is a hallmark of a wide variety of cancers. Previous research from Green and his colleagues showed that c-Myc also drives metabolic changes following T cell activation. The metabolic reprogramming fuels proliferation of effector T cells. “Activated T cells divide every four to six hours. There is no other cell in adults that can divide that fast, not even cancer cells,” Green explained.In this study, the researchers observed several metabolic changes that arose from the way c-Myc partitioned in the cell. These metabolic changes help regulate the way the cells divide, proliferate and differentiate. In a series of experiments, researchers showed how manipulating that system could affect T cell fate following asymmetric cell division by modifying production of c-Myc. “While daughter cells of activated T cells seem to have very different fates, we showed their behavior could be altered by manipulating these metabolic and regulatory pathways to increase or decrease c-Myc levels.” Green said.
Asymmetric cell division is an important driver of other fundamental processes in cells, including early embryonic development and the self-renewal of stem cells.
“Similar control mechanisms exist in other cells that divide asymmetrically, including stem cells in the digestive and nervous systems,” he added.
Newswise —
Mapping blood flow in the brain of athletes using an advanced form of ultrasound may make it easier to more accurately recognize concussions, according to a study released today that will be presented at the American Academy of Neurology’s 68th Annual Meeting in Vancouver, Canada.
“There is growing evidence that concussions can change the blood flow in the brain,” said study author Robert Hamilton, PhD, co-founder of Neural Analytics in Los Angeles, Calif., and a member of the American Academy of Neurology. “While such changes may be detected with MRI, we believe there may be a less expensive and portable way to measure these changes with a transcranial Doppler (TCD) device.” More than one million athletes experience a concussion each year in the United States.TCD uses ultrasound to map blood flow activity in the brain. Traditionally, it has measured variables like the speed and variability (pulse) of blood flowing through the arteries. But those measurements haven’t been enough to accurately detect concussion.
For this study, researchers used an advanced version of TCD ultrasound to get a more complete picture of just how the blood moves through the middle cerebral artery, one of the three major arteries in the brain.
Researchers compared a group of 66 high school athletes in contact sports who had been recently diagnosed with a concussion to a control group of 169 high school student athletes from both contact and non-contact sports. Examples of collision sports included in the study were football, soccer, basketball, hockey, water polo and lacrosse. The non-contact sports included were cheerleading, cross country, cycling, tennis and track. Both the control and concussion groups were approximately 30 percent female.
Each of the concussed athletes had their brain blood flow measured with the advanced ultrasound headset within an average of six days after the injury. They were also given a general concussion evaluation and had their blood pressure checked.
The study found that the advanced version of TCD ultrasound was able to differentiate between healthy and concussed athletes 83 percent of the time. This is in contrast to traditional TCD ultrasound measurements like change in cerebral blood flow reactivity which differentiated between the two 60 percent of the time, average blood flow speed which differentiated 55 percent of the time and blood flow resistance which differentiated 53 percent of the time.
“This research suggests that this advanced form of ultrasound may provide a more accurate diagnosis of concussion,” said Hamilton. “While more research is needed, the hope is such a tool could one day be used on the sidelines to help determine more quickly whether an athlete needs further testing.”
“This important work provides insight into a tool that may yet prove useful in the recognition and management of concussion,” said Jeffrey Kutcher, MD, FAAN, with the The Sports Neurology Clinic in Brighton, Michigan. “The potential of having an accessible technology that detects a physiological change following brain trauma is very exciting. However, what these detected blood flow changes mean to a patient’s clinical care is still unclear.”
“This is an important area of research. Testing of the TCD technique at the sideline at the time of injury will be an important next step to determine its ultimate utility,” said Randolph S. Marshall, MD, MS, with Columbia Presbyterian Medical Center in New York and a member of the American Academy of Neurology’s Science Committee.
The study was supported by the National Institutes of Health and the National Science Foundation.
Learn more about concussion at www.aan.com/concussion, where you can access the AAN’s Sports Concussion Guideline, QuickCheck app, and other resources.
The American Academy of Neurology, an association of 30,000 neurologists and neuroscience professionals, is dedicated to promoting the highest quality patient-centered neurologic care. A neurologist is a doctor with specialized training in diagnosing, treating and managing disorders of the brain and nervous system such as Alzheimer’s disease, stroke, migraine, multiple sclerosis, brain injury, Parkinson’s disease and epilepsy.
Newswise —
PRNewswire/ -- Virginia Mason Institute, a leading lean education resource for health care organizations, just released a new improvement story that outlines how a pharmaceutical error had a profound effect on a patient, leaders and staff — and eventually the processes.
Problems Lean Solves, An Improvement Story - Medication Error Sparked Team Engagement, Innovation and the Patient Safety PursuitHow did the team uncover the systemic cause of the problem, and how did they dramatically reduce defects in the process to make sure such an event never happened again?
Click here to read how the team discovered the problem and put a long term solution in place to keep patients safe.
At Virginia Mason Institute, the lean methods we teach — and our primary source of inspiration — come from the remarkable work our colleagues do every day at Virginia Mason. Read about some of the improvement work we've created, implemented and sustained to make care dramatically better for patients, providers and staff.
How a Medication Error Spurred Team Engagement, Innovation and Patient SafetyClick here to read full improvement story.Interested in learning more? Connect with us and become an email subscriber. Click here to subscribe via our Knowledge Base.
Share on TwitterShare on LinkedIn
Share on Facebook
About Virginia Mason Institute
Virginia Mason Institute provides lean coaching and education to organizations worldwide to improve patient safety, quality and efficiency. Our certified lean experts help health care leaders embed a sustainable lean culture that produces better care and improved patient and staff satisfaction.
Contact: Elaine Riordan, Public Relations SpecialistPhone: (206) 341.1600 Email: marketing@virginiamasoninstitute.org Website: www.virginiamasoninstitute.org
Virginia Mason Institute - Transformation of Health Care (PRNewsFoto/Virginia Mason Institute)Photo -http://photos.prnewswire.com/prnh/20160413/355037
Logo -http://photos.prnewswire.com/prnh/20160112/321383LOGO
Newswise —
Scientists at the University of North Carolina (UNC) School of Medicine and Sanford Burnham Prebys Medical Discovery Institute (SBP) have identified a human (host) protein that weakens the immune response to HIV and other viruses. The findings, published today in Cell Host & Microbe, have important implications for improving HIV antiviral therapies, creating effective viral vaccines, and advance a new approach to treat cancer.
“Our study provides critical insight on a paramount issue in HIV research: Why is the body unable to mount an efficient immune response to HIV to prevent transmission?” said Sumit Chanda, Ph.D., professor and director of SBP’s Immunity and Pathogenesis Program and co-senior author of the study. “This research shows that the host protein NLRX1 is responsible—it’s required for HIV infection and works by repressing the innate immune response.”
The innate immune response works by producing a cascade of signaling chemicals (interferons and cytokines) that trigger cytotoxic T cells to kill pathogens. Increasing evidence suggests that mounting an early, potent innate immune response is essential for the control of HIV infection, and may improve the effectiveness of vaccines.
“Importantly, we were able to show that deficiencies in NLRX1 reduce HIV replication, suggesting that the development of small molecules to modulate the innate immune response may inhibit viral transmission and promote immunity to infection,” said Chanda. “We anticipate expanding our research to identify NLRX1 inhibitors.”How NLRX1 reduces innate immunity to HIV
Although HIV is a single-stranded RNA virus, after it infects an immune cell it’s rapidly reverse transcribed into DNA, increasing the level of DNA found in the fluid portion of a cell (cytosol). Elevated cytosolic DNA triggers a sensor called STING (stimulator of interferon genes) that turns on the innate immune response.
“Until now, the mechanism by which NLRX1 promoted HIV infection was unexplored. We have shown that NLRX1 interacts directly with STING, essentially blocking its ability to interact with an enzyme called TANK-binding kinase 1 (TBK1),” said Haitao Guo, Ph.D., senior postdoctoral research associate in the laboratory of Jenny Ting, Ph.D., a University of North Carolina Lineberger Comprehensive Cancer Center member, the William R. Kenan Jr. Professor of Microbiology and Immunology at the UNC School of Medicine and lead author of the study. “The STING-TBK1 interaction is a critical step for interferon production in response to elevated cytosolic DNA, and initiates the innate immune response.”
“This research expands our understanding of the role of host proteins in viral replication and the innate immune response to HIV infection, and can be extended to DNA viruses such as HSV and vaccinia,” added Guo.
Relevance to cancer
“Our discovery that NLRX1 reduces the immune response to HIV is similar to the discovery of host immune checkpoints, such as PD-L1 and CTLA-1, that control the immune response to cancer,” said Ting, co-senior author of the study.
Immune checkpoints are immunological “brakes” that prevent the over-activation of the immune system on healthy cells. Tumor cells often take advantage of these checkpoints to escape detection of the immune system. Several FDA-approved drugs that target checkpoints, called checkpoint inhibitors, are now available to treat certain cancers.
“Checkpoint inhibitors have made a huge impact on cancer treatment, and significant investment by the biotech/pharmaceutical sector is being made to identify STING inhibitors as the next generation of immune-oncology therapeutics,” said Ting. “This study, showing that NLRX1 is a checkpoint of STING, sheds more light on the topic and will help advance those efforts.”
# # #
Newswise —
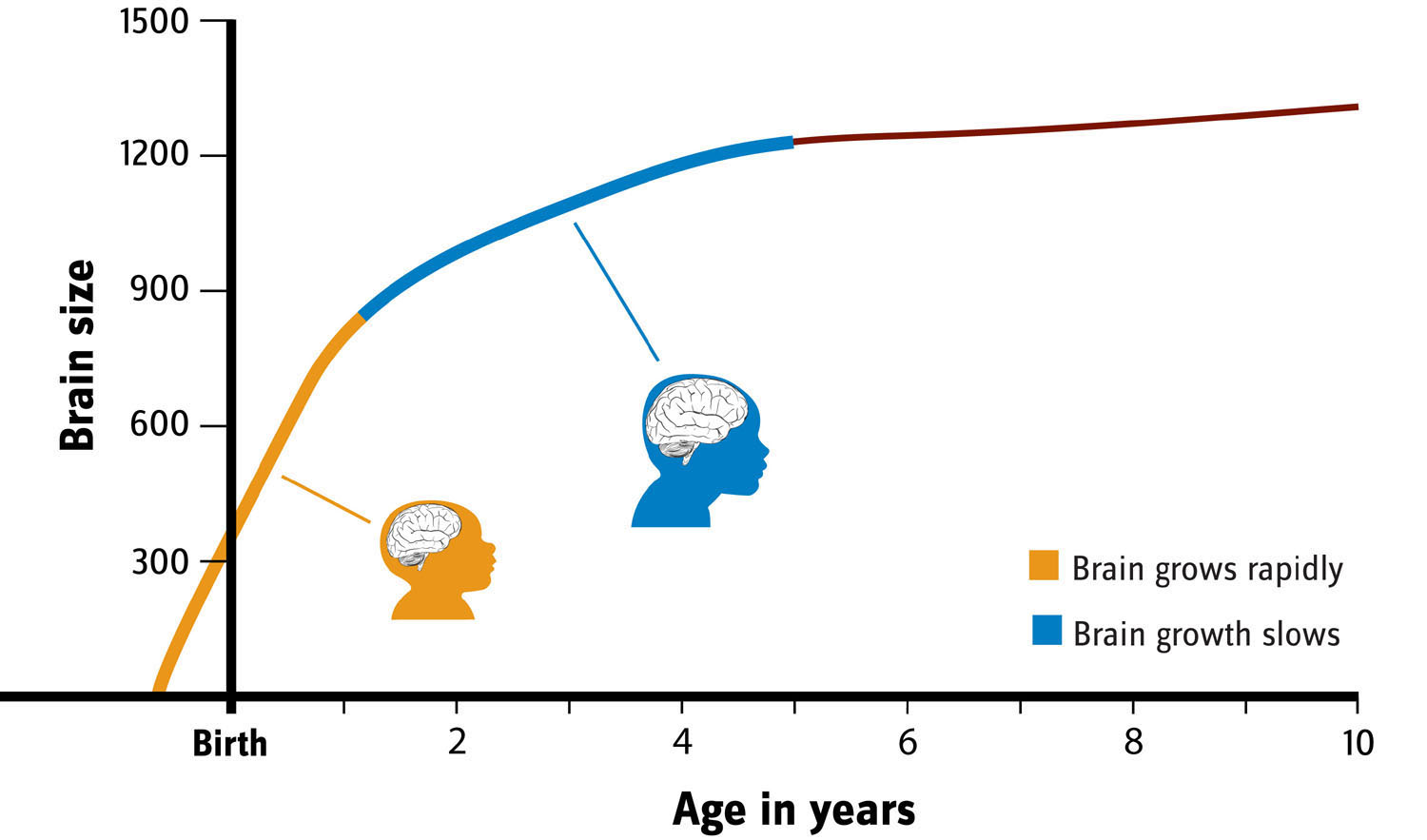
Want to know if your child’s height and weight are on track? Check the growth chart that the doctor gives you after each yearly checkup. Want to know if your child’s brain is on track for healthy attention abilities? Someday, your doctor might have a growth chart for that too.
New research from the University of Michigan Medical School suggests that it might be possible to create a growth chart of brain networks that could identify early signs of attention difficulties and, potentially, attention deficit hyperactivity disorder.
The team created the experimental growth chart by mapping the development of brain networks in more than 500 children and teens. They found networks are underdeveloped in those who have attention difficulties.
While it’s far too soon to start offering such charting to families, future development of the technique could mean better chances for children to get a firm diagnosis of ADHD sooner. It could also help track whether their ADHD treatment is improving their attention functioning, which can help them in school and life.
Growth charts as biomarkers
The research, published in JAMA Psychiatry, shows the potential for brain imaging “biomarkers” for attention problems. But the idea could extend to other psychological conditions.
Traditional growth charts show a child’s height and weight as points on curves that are based on data from hundreds of thousands of other children, and indicate normal, near-normal and problematic development.
“Growth charts enable a family and their physician to quickly spot problematic development, and when necessary, intervene appropriately,” said team leader and U-M psychiatrist Chandra Sripada, M.D., Ph.D. “In the future, we want to provide clinicians with the same sort of guidance about brain development that we can about things like height and weight.”
Maturing networks
The researchers launched the growth-charting research after noticing a gap in the state of the science.
Lead author Daniel Kessler explains, “We knew that the ability to sustain attention for an extended time increases dramatically during childhood and adolescence. We also knew that over the same time period, there are big changes in brain networks involved in attention. We came up with the idea of growth charting as a way to test if these two patterns were related: Would children with underdeveloped brain networks also have more difficulty with attention?”
Along with colleague Michael Angstadt, MAS, the researchers used data from 519 children and teens who had genetic testing, brain imaging and tests of their cognitive development as part of the Philadelphia Neurodevelopmental Cohort based at the University of Pennsylvania.
The researchers created growth charts that reflected the configuration of what are called intrinsic connectivity networks -- important units of functional brain organization. The way these networks interact may hold the key to healthy attention.
For example, one called the default mode network seems to be involved in daydreaming and inwardly focused thought, whereas another set of networks are involved in cognitively demanding tasks.
As we grow from children into adults, these two systems become more defined and separate, working in tandem like pistons: when one is on, the other turns off. But in children and those with attention difficulties, the “pistons” often misfire: the default mode network turns on and interrupts the other networks thereby interrupting attention.
The researchers who gathered the data that the growth chart is based on measured attention functioning using a standard test in which children had to respond to a sequence of letters and numbers on a computer screen. The Michigan researchers then compared the brain development seen on the scans to attention functioning. It turned out they could actually predict how well a child would do on the attention test based on their place on (or off) the brain network growth chart. The children with ADHD symptoms, and those with the lowest performance for their age on the attention tests, were the furthest off the curve of brain network development.
“These brain network growth charts show real promise,” said Sripada. “But they are far away from being ready for clinical use.”
Future research paths
The research used advanced MRI imaging, but Sripada and his colleagues hope to develop ways to track network maturity using less-expensive techniques such as electroencephalography, or EEG.
They’re working with other U-M researchers, led by Mary Heitzeg, Ph.D., and Robert Zucker, Ph.D., to see if the growth charting method will be useful in the Adolescent Brain Cognitive Development study (ABCD for short) that will involve 10,000 teens over several years.
“The ABCD study is unprecedented in size and provides a real chance to develop definitive growth charts for brain networks,” explained Sripada. “We have the opportunity to understand how brain network development relates to a variety of outcomes, including cognition, emotion, personality, and behavior.”