News
Newswise —
The discovery of long non-coding RNA (lncRNA) has dramatically changed the understanding of the biology of diseases such as cancer. The human genome contains about 20,000 protein-coding genes – less than 2 percent of the total – but 70 percent of the genome is made into non-gene-encoding RNA.
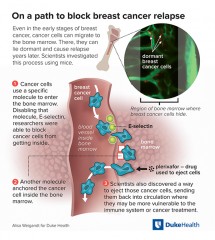
Take triple-negative breast cancer (TNBC), an aggressive subtype with poor clinical outcome, for example. Genomic studies of TNBC to crack its tough-to-treat status have mainly focused on protein-coding genes and the function of non-coding genes is still largely unknown. Using a clinically guided genetic screening approach, researchers from the Perelman School of Medicine at the University of Pennsylvania identified LINP1, a lncRNA. This lncRNA is overexpressed in triple-negative breast cancer cells and regulated by the tumor suppressor p53 and the activated cell surface protein, EGFR. LINP1 enhances the repair of DNA breaks by serving as a scaffold that links two other proteins in the repair machinery.
A BRCA1 mutation is associated with a higher risk for TNBC, which represents about 10 to 20 percent of all breast cancer cases. TNBC test negative for both the estrogen and progesterone receptors and the cell surface receptor Her2, hence its name. Since hormones are not supporting growth, the cancer is unlikely to respond to hormonal therapies and medications that target HER2.
Because of these limited therapeutic targets, many cancers, including TNBCs, are typically treated with surgery and a combination of radiation and chemotherapy that induce various types of DNA damage. However, many TNBC patients are resistant to these combination therapies. With support from the Basser Center for BRCA at Penn, the team was led by senior authors Lin Zhang, MD, the Harry Fields Associate Professor of Obstetrics and Gynecology, Chi V. Dang, MD, PhD, director of the Abramson Cancer Center, and first author Youyou Zhang, MD, PhD, a postdoctoral fellow in the department of Obstetric and Gynecology. They published their findings this week in Nature Structural & Molecular Biology. Recent studies, including publications from the Penn group, have identified lncRNAs with tumor suppressive and oncogenic activities in cancers.
Building BridgesThe two repair scaffold proteins, Ku80 and DNA-PKcs, that LINP1 links coordinate the non-homologous end-joining (NHEJ) repair molecules that fix double-strand breaks in DNA. Importantly, the team found that blocking LINP1 significantly increases sensitivity by the tumor cells to radiation therapy.
The NHEJ pathway, which repairs double-strand breaks in DNA, is one of the major pathways in tumor cells that respond to radiation treatment and chemotherapeutic agents. Inhibition of the NHEJ pathway has been proposed by oncology researchers to synergize DNA-damaging therapies for better treatment outcomes for TNBCs.
“Given the important role of LINP1 in the NHEJ pathway, our study indicates that this new class of cancer-driver gene -- the lncRNAs -- may serve as unique therapeutic targets and novel biomarkers in cancer,” Zhang said. “Collectively, our study provides new insight into the DNA damage repair pathway, long non-coding RNAs, and triple-negative breast cancer.”
Qun He, Zhongyi Hu, Yi Feng, Lingling Fan, Zhaoqing Tang, Jiao Yuan, Weiwei Shan, Chunsheng Li, Xiaowen Hu, Janos L Tanyi, Yi Fan, Qihong Huang, and Kathleen Montone, all from Penn, are coauthors.
The research was also supported by the National Institutes of Health (R01CA142776, R01CA190415; P50CA083638, P50CA174523, R01CA148759, R01NS094533), the Breast Cancer Alliance, the Ovarian Cancer Research Fund, the Foundation for Women’s Cancer, and the Marsha Rivkin Center for Ovarian Cancer Research.
Penn Medicine is one of the world's leading academic medical centers, dedicated to the related missions of medical education, biomedical research, and excellence in patient care. Penn Medicine consists of the Raymond and Ruth Perelman School of Medicine at the University of Pennsylvania (founded in 1765 as the nation's first medical school) and the University of Pennsylvania Health System, which together form a $5.3 billion enterprise.
The Perelman School of Medicine has been ranked among the top five medical schools in the United States for the past 18 years, according to U.S. News & World Report's survey of research-oriented medical schools. The School is consistently among the nation's top recipients of funding from the National Institutes of Health, with $373 million awarded in the 2015 fiscal year.
The University of Pennsylvania Health System's patient care facilities include: The Hospital of the University of Pennsylvania and Penn Presbyterian Medical Center -- which are recognized as one of the nation's top "Honor Roll" hospitals by U.S. News & World Report -- Chester County Hospital; Lancaster General Health; Penn Wissahickon Hospice; and Pennsylvania Hospital -- the nation's first hospital, founded in 1751. Additional affiliated inpatient care facilities and services throughout the Philadelphia region include Chestnut Hill Hospital and Good Shepherd Penn Partners, a partnership between Good Shepherd Rehabilitation Network and Penn Medicine.
Penn Medicine is committed to improving lives and health through a variety of community-based programs and activities. In fiscal year 2015, Penn Medicine provided $253.3 million to benefit our community.
Newswise —
Researchers have known for more than a decade that the risk of heart disease and stroke increases when people take pain relievers like ibuprofen and other non-steroidal anti-inflammatory drugs, or NSAIDs. Now, scientists from the University of California, Davis, have uncovered some of the reasons why these drugs can harm heart tissue.
The study was recently published online in the Journal of Molecular and Cellular Cardiology.
Working with heart cells from rats and mice, the team found that NSAIDs:
∙ Attack mitochondria, reducing the cardiac cell’s ability to produce energy;∙ Cause the production of reactive oxygen species, which stresses heart cells and is associated with many diseases, including heart disease;∙ Impair the cardiac cell’s proteasome, the mechanism for degrading harmful proteins. This leads to toxic buildup and eventually to the death of cardiac cells.
“We knew these non-steroidal anti-inflammatories had negative side effects for heart disease and stroke risk, “ said corresponding author Aldrin Gomes, a UC Davis associate professor of Neurobiology, Physiology and Behavior. “But now we have an idea of some of the mechanisms behind it.”
Drugs affect cardiac cells
The scientists compared naproxen, considered the safest available NSAID and available over the counter, with another, more potent anti-inflammatory, the prescription drug meclofenamate sodium. They found that:
∙ The prescription drug was more likely to negatively impact heart health than naproxen.∙ Naproxen did not affect proteasome function or cause heart cells to die. It did, however, impair mitochondrial function and increase reactive oxygen species produced in cardiac cells. It also is associated with an increase in the chance of stroke.∙ Meclofenamate sodium increased reactive oxygen species, impaired mitochondrial function, decreased proteasome function, and increased cardiac cell death.∙ “We were surprised to see that many of the NSAIDs we tested were causing the cardiac cell to die when used for prolonged periods,” said Gomes. “Some people are taking these drugs too often, and this is a problem. These drugs are abused.”Vitamin C may help decrease risk
The study results suggest that ingesting an antioxidant, like vitamin C, before taking a NSAID may prevent cardiac cell death without interfering with the drug’s ability to provide pain relief.
Gomes said that, for moderate pains, rubbing the anti-inflammatory topically onto the pained area can be effective without exposing the entire body to increased cardiovascular risk. Yet he advised caution when using NSAIDs either topically or orally.
The study was funded by the University of California and a Hellman Fellowship.
Newswise —
As we better understand the role food plays in our overall health and wellbeing, the closer the connection becomes between nutrition and medicine. Malnutrition is a critical public health problem, affecting many people across the United States and around the world. Unfortunately, the modern day manifestations of hunger are increasingly complex. In an effort to explore this evolving landscape, the May issue of the Journal of the Academy of Nutrition and Dietetics offers insights from leading registered dietitian nutritionists and other health professionals, providing a comprehensive look at malnutrition.
While traditionally thought of as starvation or famine, malnutrition in the modern world is much more complicated and often affects the most vulnerable populations: children, the elderly, and the sick. With this new issue, the Academy of Nutrition and Dietetics hopes to inform its professional community and the public about the changing face of malnutrition.
“In the community in the United States it’s clear that there are plenty of food deserts where availability of quality food and nutrition is a concern,” comments Gordon Jenson, PhD, MD, Department Head and Professor of Nutritional Sciences at Penn State University in an interview conducted by Journal of the Academy of Nutrition and Dietetics Editor-in-Chief Linda G. Snetselaar, PhD, RDN, LD. We’re dealing with a challenging continuum of malnutrition within the community setting today that is far more than classic undernutrition and starvation. It really is a continuum of individuals afflicted with disease, with injuries, in social isolation, or with limited resources. Ultimately this is all about how we get the appropriate resources and interventions to the individuals who need them. An integrated approach is critical with support from social services, mental health professionals, and medical care whenever appropriate.”
The issue includes original research reports and accompanying editorials focusing on different facets of modern malnutrition including establishing evidence-based nutrition practices, malnutrition in hospitals, malnutrition in a rapidly increasing elderly population, inflammation and its relationship to malnutrition, and developing workflows for the identification of malnutrition in a clinical setting.
An interview with past Academy president Susan Finn, PhD, RD, FAND, who served on the National Hunger Commission, provides a behind-the-scenes look at the National Commission on Hunger Report to Congress from the perspective of a registered dietitian nutritionist on the Commission. Dr. Finn and her colleagues delivered their final report to Congress in January 2016 and their findings will help guide policy makers on how to improve government programs. In the interview, Dr. Finn offered several findings from the report that can help Academy members in the fight against malnutrition:
• Focus special attention on nutrition outreach for people with disabilities, seniors, military family, and families with small children.• Support nutrition pilot programs that can yield innovative solutions.• Engage with members of Congress by responding to Action Alerts.• Become active in advocacy efforts to reduce food insecurity at the community level.• Share information on nutrition programs available in your area and encourage partnerships to improve food security.
Nutrition is now an integral part of medical treatment of disease. For example, within the last decade enteral feeding has become more routine than parenteral feeding for nutrition support among hospital patients and there is growing evidence for the effective modulation of inflammatory response with nutrients.
Addressing malnutrition in hospitals, the issue offers several resources for ameliorating the problem. The article “Building a Connection between Senior Hunger and Health Outcomes” highlights the challenges presented by the hospitalization of malnourished elderly patients. Lead investigator Stefanie Winston Rinehard, JD, MPH, Director, Department of Health and Human Services Legislation and Policy, explains, “Malnutrition affects an estimated 30% to 50% of adult hospitalized patients in the United States, but only 3.2% of these patients are discharged with a diagnosis of malnutrition. Malnourished patients have worse health outcomes when compared with well-nourished patients, including increased physician visits, longer hospital stays and readmissions, decreased function and quality of life, and increased health care costs.”
Other articles focus on the task of diagnosing malnutrition in hospital patients. “Diagnosing Malnutrition: Where Are We and Where Do We Need to Go?” discusses how accurate nutritional assessments are not always successfully integrated into clinical workflows. “Malnutrition is the skeleton in the hospital closet that continues to haunt us,” notes author Charlene Compher, PhD, RD, LDN, FADA, FASPEN. “Following decades of reports describing the prevalence and influence of malnutrition on hospital outcomes, we have seen a renewed interest in defining and classifying malnutrition.”
As the relationship between nutrition and medicine continues to develop, the Academy hopes that this collection of articles can renew the conversation about malnutrition and help practitioners better understand ways to combat hunger in their professional lives. “In past years, the ethical debate involving nutrition was primarily related to terminal or irreversible illness and the withdrawal of artificial nutrition,” emphasizes Louise Merriman, MS, RD, CDN, Director, Clinical Nutrition, New York Presbyterian Hospital, co-author of “Implementing the Care Plan for Patients Diagnosed with Malnutrition—Why Do We Wait.” “Now, with malnutrition finally recognized to be prevalent and problematic in hospitalized patient populations, the ethical debate is shifting as we ask ourselves and our team members: Why do we wait?”
Newswise —
Why does one person who tries cocaine get addicted, while another might use it and then leave it alone? Why do some people who kick a drug habit manage to stay clean, while others relapse? And why do some families seem more prone to addiction than others?
The road to answering these questions may have a lot to do with specific genetic factors that vary from individual to individual, a new study in rats suggests.
Of course, an animal study can’t explain all the factors that contribute to differences in addiction among humans. But the findings reveal new information about the roles played by both inherited traits and addiction-related changes in the brain.
The study was just published in the Proceedings of the National Academy of Sciences by a University of Michigan Medical School team.
It’s the first time scientists have shown in selectively bred animals that the propensity for addiction is linked to differences in expression of genes for specific molecules in a specific brain region. It’s also the first demonstration that a DNA tag called an epigenetic marker can predispose an individual to addiction and relapse.
Pleasure receptor DNA differences
The researchers looked in rats’ brains for the genetic instructions needed to make a key “pleasure receptor”, called D2, that allows brain cells to receive signals sent by the brain chemical dopamine – or cocaine. They found that more addiction-prone rats had lower levels of D2 instructions to begin with, compared with other rats, in an area of the brain known to play a major role in addiction.
The addiction-prone rats also were more likely to carry a specific mark on their DNA called an epigenetic tag. This tag, called H3K9me3, kept their brain cells from reading the gene for D2 receptors.
But after they became hooked on cocaine, the addiction-prone rats had the same levels of D2 as the less addiction-prone ones. And when the cocaine was taken away for a while, these rats were more likely to relapse to addictive behavior if they had started out with the epigenetic tag that kept their cells from reading the D2 gene.
Meanwhile, a comparison group of rats didn’t show signs of addiction, and didn’t relapse following abstinence.
The scientists found that these “addiction-resilient” rats started out with lower levels of instructions for making a different brain molecule also known to play a role in addiction, called FGF2. They were also more likely to carry an epigenetic mark that kept them from reading the FGF2 gene. And this might have helped protect them from becoming addicted.
“Because we had access to these rats that were bred for certain traits, and were able to control for environmental factors, such as the amount of drug exposure, we could assess differences in the brain both before and after the rats became addicted,” says Shelly Flagel, Ph.D., lead author of the new study and an assistant professor of psychiatry at U-M. “By studying their gene expression and epigenetics, as well as their response to drug availability and drug-related cues, we can link these differences in the brain to addiction-like behaviors, such as relapse. This allows us to hone in on the biology of addiction even further.”
And that kind of understanding could be a model to help the broader understanding of addiction in humans as well, Flagel says. The more that addiction is seen as having biological roots and origins in genetic traits that are inherited through families or amplified by drug taking, the better treatment options and public policy around drugs and drug users can be, she hopes.
A tale of two rat breeds
The findings come from studies of two special breeds of rats. Raised for dozens of generations in the lab of senior author Huda Akil, Ph.D., at the U-M Molecular and Behavioral Neuroscience Institute under carefully controlled conditions, the two breeds act as a way to study the effects of genetic and inherited traits on addiction-related behaviors.
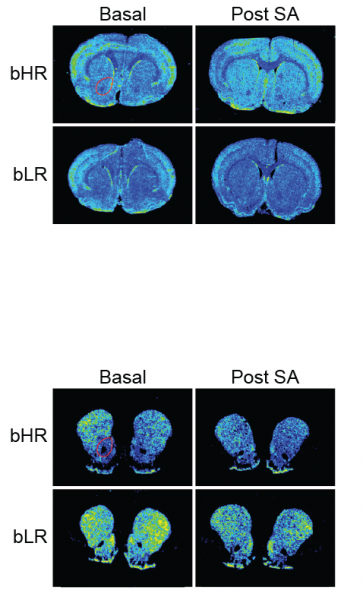
One breed, called bHR for bred high responders, tends to explore and seek novelty. The other, called bLR for bred low responders, does not. In fact, bLR rats often act anxious when presented with new situations, and prefer enclosed spaces even when they can see food in an open area.
The two breeds allow scientists to study the impact of drug use and addiction on gene expression and epigenetics in the nucleus accumbens – the brain’s “pleasure center”, where response to drugs like cocaine occurs. Normally, the dopamine system in this area responds to naturally pleasant experiences and prompts us to pursue them again. It’s as if the drug hijacks the system that fuels normal enjoyment or reward. And that can make the usual goal-driven motivated behavior that’s driven by pleasure go awry.
In the new study, the scientists first trained all the rats to expect to find cocaine in certain places, to poke their nose into a hole to get a controlled dose of it, and to expect it would be available when a certain light was shining. Even the anxious, timid bLR rats learned to take the drug.
Although both groups of rats took the same amount of drug, the two breeds differed dramatically in how likely they were to seek out cocaine repeatedly. The bHR rats were much more likely to keep seeking cocaine, even when it was not available.
After a week without cocaine, bHR rats were more likely to ‘relapse’ after getting an injection of cocaine. After a month with no cocaine, bHRs were much more likely than bLRs to start seeking it again when the light previously associated with cocaine delivery started coming on again. This is similar to what humans recovering from addiction often report: their craving for drugs returns when they see drug paraphernalia or return to a place where they once got or took drugs.
“It is likely that the propensity to seek drugs and become addicted to them involves numerous genes. Moreover, factors beyond novelty-seeking including stress and depression can lead to substance use in some individuals,” says Akil. She, Flagel and their colleagues are now using broad-based genotyping to uncover other genes that contribute to various facets of drug abuse and addiction. These genetic findings will point to potential biomarkers and more targeted treatment strategies for substance use disorders.
Newswise —
The debilitating pain and disability of migraine also attacks the emotional, social and financial fabric of a family, according to a new study conducted by researchers at Montefiore Headache Center, Albert Einstein College of Medicine, affiliated with the Uniformed Services University of the Health Sciences, Vedanta Research, the Mayo Clinic and Allergan plc. The findings were published today in Volume 91, Issue 5 ofMayo Clinic Proceedings.
The Chronic Migraine Epidemiology and Outcomes (CaMEO) Study surveyed 4,022 people with migraine as well as their spouses or domestic partners to gain a full picture of the effect of migraine on the family. Approximately 41% of people with migraine and 23% of spouses stated that they believed those impacted by migraine would be better parents if they did not have migraine, which consequently led to half of migraineurs missing at least one family activity in the past month. Approximately one-third of people with migraine and 21% of their spouses/partners endorsed worries about long-term financial security for their family due to migraine. Perceived burden was the greatest among people with chronic migraine (migraine with headache on 15 or more days per month) and among those with more frequent attacks.
“This study highlights the significant burden that migraine can have on a wide range of family activities, parenting responsibilities, spousal relationships and family finances,” said study lead author Dawn C. Buse, Ph.D., director of Behavioral Medicine, Montefiore Headache Center and associate professor of neurology at Albert Einstein College of Medicine. “Respondents with migraine and their partners noted a great deal of emotional distress related to how this condition affects their family member including guilt, worry and sadness. These findings underscore the challenges and negative impact that people with migraine and their family members’ experience.”
The CaMEO Study is a U.S. web-panel study that gathered information on the perceived impact of migraine—episodic or chronic-- on people with migraine, their partners and their children by surveying each of the three types of respondents from September 2012 to November 2013. As the study authors point out, an accurate diagnosis and appropriate treatment are essential to reducing the overall burden of migraine.
“The consequences of migraine can be devastating and far-reaching for people with migraine and their families,” said Richard B. Lipton, M.D., director of Montefiore Headache Center and vice chair of neurology, and the Edwin S. Lowe Chair in Neurology, Albert Einstein College of Medicine. “As a next step, we are analyzing responses from the children of those with migraine, who are 13 and older. We are also developing the “Impact of Migraine on Partners and Children Scale (IMPACS)” to help quantify the family burden of migraine. We hope that improved diagnosis, treatment and enhanced recognition of the burden associated with migraine leads to better outcomes for all family members,” concluded Dr. Lipton, who is the study Primary Investigator.
Additional study authors include Ann I. Scher, Ph.D., Uniformed Services University of the Health Sciences, David W. Dodick, M.D., Mayo Clinic in Phoenix Arizona, Michael L. Reed, Ph.D., Vedanta Research, Kristina M. Fanning, Ph.D., Vedanta Research, Aubrey Manack Adams, Ph.D., Allergan plc and Richard B. Lipton, M.D., Montefiore/Einstein.
Funding for the Chronic Migraine Epidemiology and Outcomes (CaMEO) study was provided by Allergan plc.
About Montefiore Health SystemMontefiore Health System is one of New York’s premier academic health systems and is a recognized leader in providing exceptional quality and personalized, accountable care to approximately three million people in communities across the Bronx, Westchester and the Hudson Valley. It is comprised of 10 hospitals, including the Children’s Hospital at Montefiore, Burke Rehabilitation Hospital and close to 200 outpatient care sites. The advanced clinical and translational research at its’ medical school, Albert Einstein College of Medicine, directly informs patient care and improves outcomes. From the Montefiore-Einstein Centers of Excellence in cancer, cardiology and vascular care, pediatrics, and transplantation, to its’ preeminent school-based health program, Montefiore is a fully integrated healthcare delivery system providing coordinated, comprehensive care to patients and their families. For more information please visit www.montefiore.org. Follow us on Twitter and view us on Facebook and YouTube.
About Albert Einstein College of MedicineAlbert Einstein College of Medicine is one of the nation’s premier centers for research, medical education and clinical investigation. During the 2015-2016 academic year, Einstein is home to 731 M.D. students, 193 Ph.D. students, 106 students in the combined M.D./Ph.D. program, and 278 postdoctoral research fellows. The College of Medicine has more than 1,900 full-time faculty members located on the main campus and at its clinical affiliates. In 2015, Einstein received $148 million in awards from the National Institutes of Health (NIH). This includes the funding of major research centers at Einstein in aging, intellectual development disorders, diabetes, cancer, clinical and translational research, liver disease, and AIDS. Other areas where the College of Medicine is concentrating its efforts include developmental brain research, neuroscience, cardiac disease, and initiatives to reduce and eliminate ethnic and racial health disparities. Its partnership with Montefiore Medical Center, the University Hospital and academic medical center for Einstein, advances clinical and translational research to accelerate the pace at which new discoveries become the treatments and therapies that benefit patients. Through its extensive affiliation network involving Montefiore, Jacobi Medical Center—Einstein’s founding hospital, and three other hospital systems in the Bronx, Brooklyn and on Long Island, Einstein runs one of the largest residency and fellowship training programs in the medical and dental professions in the United States. For more information, please visit www.einstein.yu.edu, read our blog, follow us on Twitter, like us on Facebook, and view us on YouTube.
Newswise —
Groundhog Day 1994 is one Linda Friedrich will never forget. That’s the day a neurologist told her, “You have multiple sclerosis and there’s nothing we can do.”The youngest of her three children was only 2 years old, she recalled, and her only vision of MS was a relative who could no longer walk or talk.Luckily, she got the new drug, Betaseron, within four months of her diagnosis and has experienced only a couple of recurrences which involved numbness from the waist down. “I’ve been very fortunate,” she said, but admits, “my left leg is weaker.”However, when it came to working out in the gym, Friedrich said, “I didn’t know what I should be doing.” That’s why she jumped at the chance to participate in a South Dakota State University study to determine whether strength and flexibility training could help MS patients.
“We’re looking at how we can improve function and, at the same time, quality of life,” said study director Bradley Bowser. He is director of the biomechanics laboratory and an assistant professor in the SDSU Department of Health and Nutritional Sciences. He began working with MS patients in 2007 as part of his doctoral research at the University of Georgia.
Though research has shown that exercise can improve strength and balance for those with Parkinson’s disease, Bowser said, “Not a lot has been done in this area with those who have MS, because the disease is not homogenous. Everyone has different symptoms—one person has weakness in one leg, another blurred vision. It depends on where MS attacks the nervous system.”
Simple daily living activities, such as handwashing, can become difficult for MS patients due to balance issues, explained Bowser. “Because of problems with balance and instability, MS patients may become less physically active and, thus, more susceptible to illnesses due to a sedentary lifestyle.”
How leg weakness affects movementWhen Bowser analyzed the results of a previous study done as part of his doctoral work at the University of Georgia, he found that the participants with MS who exhibited leg weakness took longer to move from a sitting to a standing position than those with MS who had leg strength comparable to the healthy control group. However, it was how that weakness affected their movement that was most striking.Those with leg weakness displayed greater trunk flexion and were thrusting their upper bodies forward quickly to create the momentum they needed to compensate for decreased leg extensor strength, he explained. The combination of flexion and thrust places additional stress on the lower back, thus increasing the risk of injury.
Measurements showed that MS patients with normal leg strength and the control group had more than 38 percent greater leg extensor strength than those experiencing leg weakness. Less leg strength, in turn, decreased their knee extensor power, he explained. These findings were published last year in Clinical Biomechanics.In addition, Bowser looked at symmetry and stability during dynamic movement comparing the healthy control group with the MS group before and after the intervention. Preliminary results showed that resistance and flexibility training improved balance and symmetry.Looking at exercise, behavioral therapyBowser’s most recent study, which began last summer, will further examine whether resistance, stability and flexibility training can improve balance and other functional movements for people diagnosed with MS. In addition, the researchers will look at whether cognitive behavioral therapy can provide additional benefits for MS patients. The research is funded through grants from the Women and Giving Program at the SDSU Foundation and the SDSU Research and Scholarship Support Fund.
During the 10-week intervention, all participants did strength, balance and flexibility training for one hour twice a week to strength their muscles and improve their balance. However, half the participants also completed a one-hour cognitive behavioral therapy session each week. During the therapy sessions, participants were asked to set specific behavioral goals, which could include exercise. In addition, behavioral therapy can help clients understand their thoughts and feelings, including coping with depression and anxiety. The study is concluding and results are being analyzed.
Friedrich, who was part of the exercise-only group, said, “I felt good afterward. I might have MS but I can still do this.” Her weaker left leg improved but then reached a plateau, she said, “but my right leg and upper body strength kept going.”
She also noted improvements in balance. Before the training, she pointed out, “if I caught my foot on a rug, I’d be down. Now, I can catch myself and I don’t fall.”
For Friedrich, keeping up with her family is important. “My goal was to walk up Harney Peak when our family went to the Black Hills and I did.”
Newswise —
What if a map of the brain could help us decode people's inner thoughts?
Scientists at the University of California, Berkeley, have taken a step in that direction by building a "semantic atlas" that shows in vivid colors and multiple dimensions how the human brain organizes language. The atlas identifies brain areas that respond to words that have similar meanings.
The findings, to be published April 28, 2016 in the journalNature, are based on a brain imaging study that recorded neural activity while study volunteers listened to stories from the "Moth Radio Hour." They show that at least one-third of the brain's cerebral cortex, including areas dedicated to high-level cognition, is involved in language processing.
Notably, the study found that different people share similar language maps: "The similarity in semantic topography across different subjects is really surprising," said study lead author Alex Huth, a postdoctoral researcher in neuroscience at UC Berkeley.
Detailed maps showing how the brain organizes different words by their meanings could eventually help give voice to those who cannot speak, such as victims of stroke or brain damage, or motor neuron diseases such as ALS.
While mind-reading technology remains far off on the horizon, charting how language is organized in the brain brings the decoding of inner dialogue a step closer to reality, the researchers said.
For example, clinicians could track the brain activity of patients who have difficulty communicating and then match that data to semantic language maps to determine what their patients are trying to express. Another potential application is a decoder that translates what you say into another language as you speak.
"To be able to map out semantic representations at this level of detail is a stunning accomplishment," said Kenneth Whang, a program director in the National Science Foundation's Information and Intelligent Systems division. "In addition, they are showing how data-driven computational methods can help us understand the brain at the level of richness and complexity that we associate with human cognitive processes."
Huth and six other native English-speakers served as subjects for the experiment, which required volunteers to remain still inside the functional Magnetic Resonance Imaging scanner for hours at a time.
Each study participant's brain blood flow was measured as they listened, with eyes closed and headphones on, to more than two hours of stories from the "Moth Radio Hour," a public radio show in which people recount humorous and/or poignant autobiographical experiences.
Their brain imaging data were then matched against time-coded, phonemic transcriptions of the stories. Phonemes are units of sound that distinguish one word from another.
That information was then fed into a word-embedding algorithm that scored words according to how closely they are related semantically.
The results were converted into a thesaurus-like map where the words are arranged on the flattened cortices of the left and right hemispheres of the brain rather than on the pages of a book. Words were grouped under various headings: visual, tactile, numeric, locational, abstract, temporal, professional, violent, communal, mental, emotional and social.
Not surprisingly, the maps show that many areas of the human brain represent language that describes people and social relations rather than abstract concepts.
"Our semantic models are good at predicting responses to language in several big swaths of cortex," Huth said. "But we also get the fine-grained information that tells us what kind of information is represented in each brain area. That's why these maps are so exciting and hold so much potential."
"Although the maps are broadly consistent across individuals, there are also substantial individual differences," said study senior author Jack Gallant, a UC Berkeley neuroscientist. "We will need to conduct further studies across a larger, more diverse sample of people before we will be able to map these individual differences in detail."
###
Newswise —
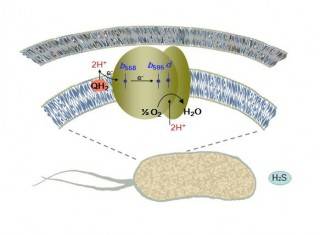
An international team of including the Lomonosov Moscow State University researchers discovered which enzyme enables Escherichia colibacterium (E. coli) to breathe. The study is published in theScientific Reports.
Scientists discovered how the E. coli bacterium can survive in the human gut - earlier the question how they breathe was a mystery to experts. Vitaliy Borisov, Senior Researcher, Doctor of Biological Sciences, Professor of the Russian Academy of Sciences, A.N. Belozersky Research Institute physical and chemical biology employee, the Lomonosov Moscow State University and one of the authors, explains that breathing E. coli uses special enzymes, which are absent in the human body. This means that the discovery of the scientists can contribute to the creation of new drugs, which will be detrimental to the bacteria without harming a human.
The energy for the vital activity of any organism comes from food, and is generated by the means of redox processes in the body. The food is converted into energy not directly but through intermediaries. First, the complex molecules are decomposed into simpler: proteins are decomposed into amino acids, fats - to fatty acids, carbohydrates - to monosaccharides. Oxidation of simpler molecules releases energy, which all is contained in the electrons.
The electrons passes to the respiratory chain with the so-called reducing equivalents (electron-carrying compound). They are NADH (nicotinamide adenine dinucleotide) and ubiquinol, also known as coenzyme Q. These two basic reducing equivalents fully cope with the processing of food: NADH is a water-soluble compound and ubiquinol is fat-soluble. Membranous enzymes accept electrons from reducing equivalents and transfer them to molecular oxygen.
The terminal cytochrome oxidase is the main membrane enzyme responsible for the human mitochondrial respiration and was thought to be used for the breath of E. coli as well. The scheme of oxidases action is simple: transferring electrons to molecular oxygen, reducing equivalents are oxidized again, and as a result "the energy currency" of the cell - the proton-moving force is generated.
'If you stop breathing, you die just because oxygen does not flow to the oxidase, and it does not produce energy,' says Vitaly Borisov.
The Escherichia coli bacterium lives in the gastrointestinal tract, where a lot of hydrogen sulfide is produced, which attenuates mitochondrial respiration. Free hydrogen sulfide inhibits cytochrome oxidase work. Its concentration exceeds several hundred times the minimum concentration required for substantial blocking of this enzyme. Hence, it seems that the E. coli bacterium cannot "breathe", but despite that the bacteria somehow survive in the intestine. The researchers assumed that the breath in the presence of hydrogen sulfide is still possible, but due to other oxidase. The fact is that the breath in people and bacteria occur in different ways. Each cell in our body "breathes" due to the work of only the cytochrome-c oxidase, others we have not. However, the E. coli bacteria has two types of oxidase: bo-type cytochrome oxidase (analogue of "human" cytochrome-c oxidase) and completely different bd-type cytochromes.
'Our hypothesis was that the bd-type oxidase (bd-I and bd-II) are more resistant to the hydrogen sulfide inhibition than the bo-type cytochrome oxidase,' commented Vitaly Borisov.
To test this hypothesis scientists needed to learn how the sulfide presence in the environment affects the growth of the E. coli bacteria cells, which have only one terminal oxidase (bd-I, bd-II or bo) in the respiratory chain. a variety of biochemical, biophysical and microbiological methods and approaches were applied, as well as the method of the intended mutagenesis.
The hypothesis was fully confirmed.
'Bo-oxidase's activity is completely inhibited by the hydrogen sulfide, while the work of the bd-oxidases remains untouched by the H2S. Thus, in order to successfully produce the main types of "the energy currency" under a high concentration of hydrogen sulfide, the intestinal microflora inhabitants should use a unique type of terminal oxidases, which is missing in the cells of humans and animals,' says Vitaly Borisov.
The discovery could be used in the future to develop medicines that regulate the intestinal microflora and relieving it from harmful bacteria. As human cells do not contain the bd-type oxidase, the question of the ability to combat disease-causing bacteria without causing harm to the human body becomes relevant. For example, the bacterium causing tuberculosis, which's primarily membrane enzyme is also a bd-type oxidase, quickly gaining resistance to classical antibiotics. Through this study there is a prospect of a new type of antibiotics "turning off" the oxygen only to the harmful bacteria cells, not to human cells.
Newswise —
Research from Ann & Robert H. Lurie Children’s Hospital of Chicago conducted in mice shows the drug hydrocortisone — a steroid commonly used to treat a variety of inflammatory and allergic conditions — can also prevent lung damage that often develops in premature babies treated with oxygen.
If affirmed in human studies, the results could help pave the way to a much-needed therapy for a bronchopulmonary dysplasia (BPD), a condition that affects 10,000 newborns in the United States each year and can lead to chronic lung disease and, ultimately, heart failure.
In a set of experiments, to be published in the May print issue of the journal Pediatric Research, a team of Lurie Children’s scientists showed the drug reduced damage to the delicate blood vessels inside the lungs of newborn mice and reversed some of BPD’s harmful downstream effects on the heart.
“Bronchopulmonary dysplasia is a devastating, often unavoidable side effect of a standard lifesaving therapy with oxygen used to treat newborn babies, so our findings are a promising indicator that a well-known drug that’s been around for a long time may help stave off some of this condition’s worst after-effects,” says study lead investigator and Lurie Children’s neonatologist Marta Perez, M.D., who is also assistant professor of Pediatrics at Northwestern University Feinberg School of Medicine.
BPD often develops in preemies as a result of oxygen treatment — a lifesaving therapy given to premature babies to ensure their brains, hearts and lungs get enough of this vital gas so they can develop and function properly. However, high levels of oxygen can also damage the delicate air sacs inside the lungs, the tiny filters that exchange carbon dioxide for oxygen.
Damaged by high levels of oxygen, these immature sacs, called alveoli, can become misshapen and reduce the lungs’ capacity to filter. Over time, the damage spreads further, as the blood vessels inside the lungs harden and develop abnormally high pressure. Persistently elevated pressure inside the lungs, a disease known as pulmonary hypertension can, over time, lead to heart failure.
Oxygen supplementation is vital for premature newborns, yet because it can have such serious side effects, scientists have long sought therapies that can avert oxygen-induced damage in premature lungs.
The new study findings show that hydrocortisone prevented the development of pulmonary hypertension and enlarged heart muscle, the two common consequences of BPD.
In a set of experiments, researchers placed a group of newborn mice in chambers with high levels of oxygen, while another group was allowed to breathe room air. Animals living in high-oxygen chambers quickly developed the mouse version of BPD, mimicking human disease. Mice with BPD were given either low or high doses of hydrocortisone or placebo. As expected, mice treated with placebo developed pulmonary hypertension and enlarged right side of the heart. However, mice treated with hydrocortisone showed near normal right heart ventricles, despite having BPD. Mice with BPD treated with placebo went on to develop abnormally thickened lung vessels, a cardinal sign of pulmonary hypertension, while mice with BPD treated with hydrocortisone had near-normal blood vessels in their lungs, the researchers found.
Next, researchers set out to find out how hydrocortisone protected the lungs of premature mice. Building on an earlier observation, the scientists focused on an enzyme called PDE-5, known to break down a signaling molecule that shields and strengthens blood vessels. In a previous study, the Lurie Children’s team found that too much oxygen can interfere with the activity of PDE-5 and thus speed up the breakdown of this vessel-shielding signaling molecule. Hydrocortisone, the new study found, protected the lung by preventing PDE-5 from going haywire despite high levels of oxygen. Comparing lung cells from mice exposed to high levels of oxygen, the researchers noticed that animals treated with steroids had far lower levels of PDE-5 than mice that didn’t get the treatment.
That finding, the team says, points to the underlying mechanism behind the drug’s protective effect.
In a final observation, the team discovered that higher doses of hydrocortisone could have the opposite effect and damage lung tissue. Indeed, when researchers examined lung tissue under a microscope, they noticed that animals treated with 10 mg of cortisone per kilogram of body weight had abnormal lung tissue. By contrast, animals given half that dose or a tenth of that dose had normal lung tissue.
“Supplemental oxygen has been our standard treatment for critically ill preemies, and while needed, it’s not without risk,” says senior author Kathryn Farrow, M.D., Ph.D., a neonatologist at Lurie Children’s and associate professor of pediatrics at Northwestern University Feinberg School of Medicine. “Our findings provide new insights and new possible pathways to mitigate or completely eliminate the damaging side effects of an otherwise lifesaving therapy.”
The work was funded by the National Institutes of Health under grant HL 109478 and the Lurie Children’s Department of Pediatrics Physician Scientist Research Award.
Co-investigators included Kamila Wisniewska, Keng Jin Lee, Herminio Cardona, and Joann Taylor, from Northwestern University Feinberg School of Medicine.
Research at Ann & Robert H. Lurie Children’s Hospital of Chicago is conducted through the Stanley Manne Children’s Research Institute. The Manne Research Institute is focused on improving child health, transforming pediatric medicine and ensuring healthier futures through the relentless pursuit of knowledge. In partnership with Northwestern University Feinberg School of Medicine, our scientists work in labs, in clinics, at the patient bedside and in the community to unravel the root causes of pediatric and adolescent disease, to understand childhood injury and to find factors that precipitate health problems in childhood and over a lifetime. Our researchers work every day to develop new therapies and prevention strategies.
Newswise —
Hearing socially meaningful sounds can change the ear and enable it to better detect those sounds, according to researchers at Georgia State University who studied the phenomenon in green treefrogs.
The findings are published in the Journal of Experimental Biology.
“The ear is modifiable,” said Walter Wilczynski, a professor in the Neuroscience Institute at Georgia State. “It’s plastic. It can change by getting better or worse at picking up signals, depending on particular types of experiences, such as listening to social signals. If frogs have a lot of experience hearing their vocal signals, the ones that are behaviorally meaningful to them, their ear changes to help them better cope with processing those signals.”
Each species has its own calls that influence social behavior. For instance, dogs bark, cats meow, frogs croak and humans speak using language. In animals, when males hear the calls of other males, they can determine if these males are getting too close in proximity or competing with them for females. When females listen to these calls, they can select the mate of their choice.
The findings could have important implications for elderly people in nursing homes or prisoners in solitary confinement, both of whom have little social interaction. Scientists already know a lack of social structure is a “huge risk factor for every neurological and psychiatric disease we know about,” but this study shows it could also have an effect on basic sensory function, Wilczynski said.
The study explored a phenomenon called forward masking, which occurs when a sound immediately precedes another sound someone is trying to hear and interferes with the ability to understand it. Because of the closeness in time between the two noises, the ear hasn’t finished processing the first signal before the second one occurs. This phenomenon can be detected with electrophysiological hearing tests.
Researchers used green treefrogs because they have a simple social system with only one or two vocal calls. The research team examined how animals detect socially meaningful sound after hearing their species’ calls for an extended period of time versus being in social isolation and only hearing random sounds. In the lab, the experimental group heard their species’ specific calls every night for 10 consecutive nights as they would in a normal social breeding chorus in the wild, while the control group heard random tones with no social meaning. Then the researchers placed electrodes on the skin near the frogs’ ears and measured the response of their ears to sound.
“What we find is that if they’ve had a lot of social stimulation, through their socially meaningful calls, the forward masking is reduced,” Wilczynski said.
In a previous study published in the journal Proceedings of the Royal Society B: Biological Sciences, the researchers found when green treefrogs heard social signals over several nights, not just random sounds, their ears were more sensitive to the amplitude (loudness) of sound and responded more robustly.
“If you have a lot of social interactions, a lot of social stimulation in the form of vocal signals, it’s actually modifying your ear and making your ear more sensitive,” Wilczynski said. “It’s making it easier to pick out signals in acoustically cluttered environments. And these are things that are not only important to frogs, which have to do this in a chorus, but to us, too.”
“My guess is people who have a lot of experience with our social vocal signal, which is our speech, this probably helps keep their sensory system in a healthy state that helps them pick out those signals,” Wilczynski said.
The researchers are unsure, however, how this change in the ear occurs or what particular change has been made, although they believe the modification occurs in the inner ear based on electrophysiological tests.
The study was led by Megan Gall, previously a post-doctoral researcher at Georgia State and now an assistant professor of biology at Vassar College.